MRI sheds light on COVID vaccine-associated heart muscle injury
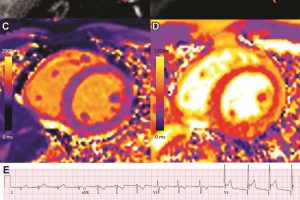
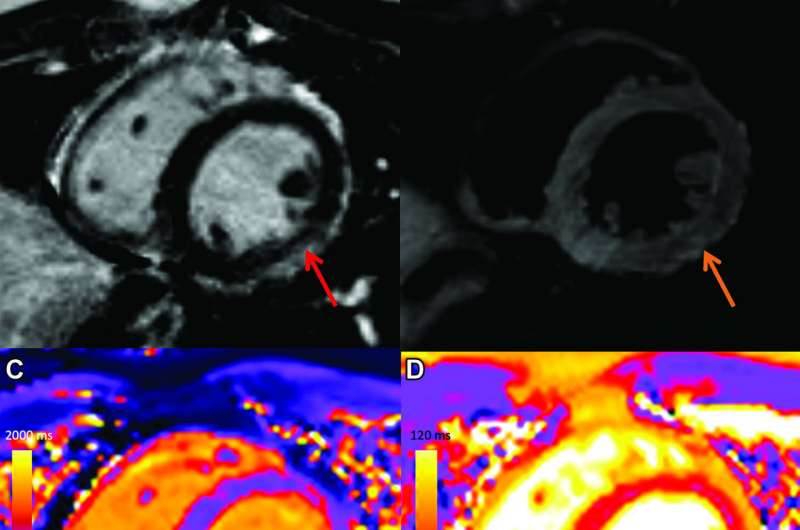
Vaccine-associated myocarditis shows a similar injury pattern on cardiac MRI compared to other causes of myocarditis, but abnormalities are less severe, according to a new study published in the journal Radiology.
Myocarditis, or inflammation of the heart muscle, often occurs as a result of a viral infection, including COVID-19. It can affect the heart’s rhythm and ability to pump blood and may leave behind lasting damage in the form of scarring of the heart muscle. Myocarditis has also been reported as a rare complication of the messenger RNA (mRNA)-based COVID-19 vaccines.
Cardiac MRI has an important role in the assessment of acute myocarditis with unparalleled ability for noninvasive characterization of myocardial tissue. Understanding the pattern and extent of myocardial injury and its implications will allow for improved care of these patients and may help to address vaccine hesitancy.
Therefore, cardiac radiologist Kate Hanneman, M.D., M.P.H., and colleagues at University Health Network, University of Toronto, set out to determine the pattern and extent of cardiac MRI findings in myocarditis associated with COVID-19 vaccination and to compare these findings to other causes of myocarditis, including COVID-19.
“We know that the risk of myocarditis following COVID-19 vaccination is very low. However, there is very limited data on the extent of injury in the heart in comparison to other causes of myocarditis,” Dr. Hanneman said.
For this retrospective study, the researchers analyzed data from 92 consecutive adult patients with myocarditis and abnormalities on cardiac MRI performed at a tertiary referral hospital between 2019 and 2021. Patients were classified into one of three groups: myocarditis following COVID-19 vaccination, myocarditis following COVID-19 illness, and myocarditis not associated COVID-19 vaccination or illness.
Of the 92 patients, 21 (22%) had myocarditis following COVID-19 vaccination (mean age 31 years). Ten patients (11%) had myocarditis following COVID-19 illness (mean age 51 years), and 61 (66%) had other myocarditis (mean age 44 years). Patients with myocarditis following vaccination were younger and more frequently male compared to the other groups.
Chest pain occurred in all 21 patients with vaccine-associated myocarditis. The pain started one to seven days after vaccination and lasted one to six days. Fourteen of the patients (67%) were admitted to hospital with a median length of stay of 3 days. No patients were admitted to the intensive care unit. Troponin levels were elevated in all patients admitted to hospital and substantially decreased in all by the time of discharge.
MRI findings in vaccine associated myocarditis included late gadolinium enhancement in 17 (81%) and left ventricular dysfunction in 6 (29%). Cardiac MRI showed that, compared with other causes of myocarditis, patients with vaccine-associated myocarditis had less functional impairment and less extensive myocardial abnormalities. Patients with COVID-19 illness and other myocarditis had a higher prevalence of abnormalities involving the interventricular septum and worse myocardial injury measured by T1 mapping.
At short-term follow-up (median 22 days), all patients with vaccine-associated myocarditis were asymptomatic with no adverse events.
“These results tell us that myocarditis following COVID-19 vaccination tends to be relatively mild and resolves quickly,” Dr. Hanneman said.
First author and cardiac imaging fellow, Matteo Fronza, M.D., said that resolution of all symptoms and lack of adverse events at follow-up is reassuring. However, longer-term follow-up is needed.
The researchers emphasized that COVID-19 illness can result in myocardial injury that is associated with adverse outcomes in hospitalized patients, and this consideration should be balanced against the low risk of vaccine-related complications.
“Not only is myocarditis following COVID-19 vaccination very rare, it also tends to be less severe than myocarditis following SARS-CoV2 infection,” Dr. Hanneman said.
Source: Read Full Article




